IVF or IVF with Genetic Testing: Choosing the Right Path

The core distinction between IVF and IVF with genetic testing is that the latter involves screening embryos for genetic abnormalities before implantation, offering higher success rates and reduced miscarriage risk.
Choosing between standard IVF and IVF with preimplantation genetic testing (PGT) depends on your medical history, age, past IVF outcomes, and personal preferences. This guide breaks down the differences, benefits, limitations, and who should consider each option.
Did you know that 1 in 3 embryos created through fertility treatments may have chromosomal abnormalities? This hidden challenge underscores why hopeful parents today face critical decisions when building their families. Understanding the differences between standard procedures and advanced screening options can significantly shape outcomes.
Traditional in vitro fertilization involves combining eggs and sperm outside the body to create embryos, which are then transferred to the uterus. A newer approach adds preimplantation genetic testing (PGT), a process that evaluates embryos for chromosomal issues before transfer. This screening aims to improve success rates and reduce risks like miscarriage.
Choosing between these paths involves balancing factors like cost, time, and emotional resilience. Some families prioritize minimizing uncertainty, while others focus on affordability or ethical considerations. This article provides a clear, unbiased comparison to help U.S.-based readers navigate their options confidently.
Comparison Table: IVF vs IVF with Genetic Testing
| Feature | IVF (Standard) | IVF with Genetic Testing (PGT) |
|---|---|---|
| Embryo Testing | No | Yes (PGT-A, PGT-M, PGT-SR) |
| Success Rate | Moderate (age-dependent) | Higher implantation & live birth rates |
| Miscarriage Risk | Higher | Significantly reduced |
| Cost | Lower | Higher due to testing fees |
| Best For | Women under 35, first IVF try | Women >35, recurrent loss, known genetics |
| Time to Transfer | Fresh cycle or Day 5 | Typically frozen after biopsy |
| Chance of Selecting a Healthy Embryo | Blind (morphology only) | Targeted (based on DNA) |
Key Takeaways
- Standard fertility treatments and embryo screening methods offer distinct paths to parenthood.
- Genetic analysis can identify chromosomal concerns early, potentially improving pregnancy success.
- Financial, logistical, and personal factors all play roles in decision-making.
- Balanced insights help families align choices with their unique priorities.
- Ethical considerations and medical guidance are central to the process.
📞 Get in Touch for a Free Surrogacy Consultation
📱 +91-8800481100 (WhatsApp | LINE | Viber)
📧 neelam@ivfconceptions.com

Understanding the Fundamentals of IVF and Genetic Testing
Many families embarking on fertility journeys encounter pivotal choices about embryo health. Two core approaches—standard lab-based fertilization and advanced screening methods—shape modern treatment paths. Grasping how these processes work lays the groundwork for informed decisions.
What is In Vitro Fertilization (IVF)?
In vitro fertilization begins with collecting eggs, which are then combined with sperm in a lab. Fertilization occurs outside the body, allowing embryos to develop in controlled conditions. These embryos are monitored for growth before potential transfer to the uterus.
An Overview of Preimplantation Genetic Testing (PGT)
Preimplantation genetic testing adds a critical layer by examining embryos for chromosomal issues. At the blastocyst stage (day 5-6), a few cells are biopsied and analyzed. This screening identifies abnormalities like Trisomy 21, helping select the healthiest options for transfer.
Unlike preimplantation genetic diagnosis (PGD), which targets specific inherited diseases, PGT focuses on broader chromosomal health. By testing embryos early, clinics aim to improve pregnancy success rates while reducing risks. Understanding these steps ensures you can weigh options with clarity as you progress.
What is IVF?
IVF (In Vitro Fertilization) is a fertility treatment in which eggs are retrieved, fertilized in a lab with sperm, and the resulting embryos are transferred into the uterus.
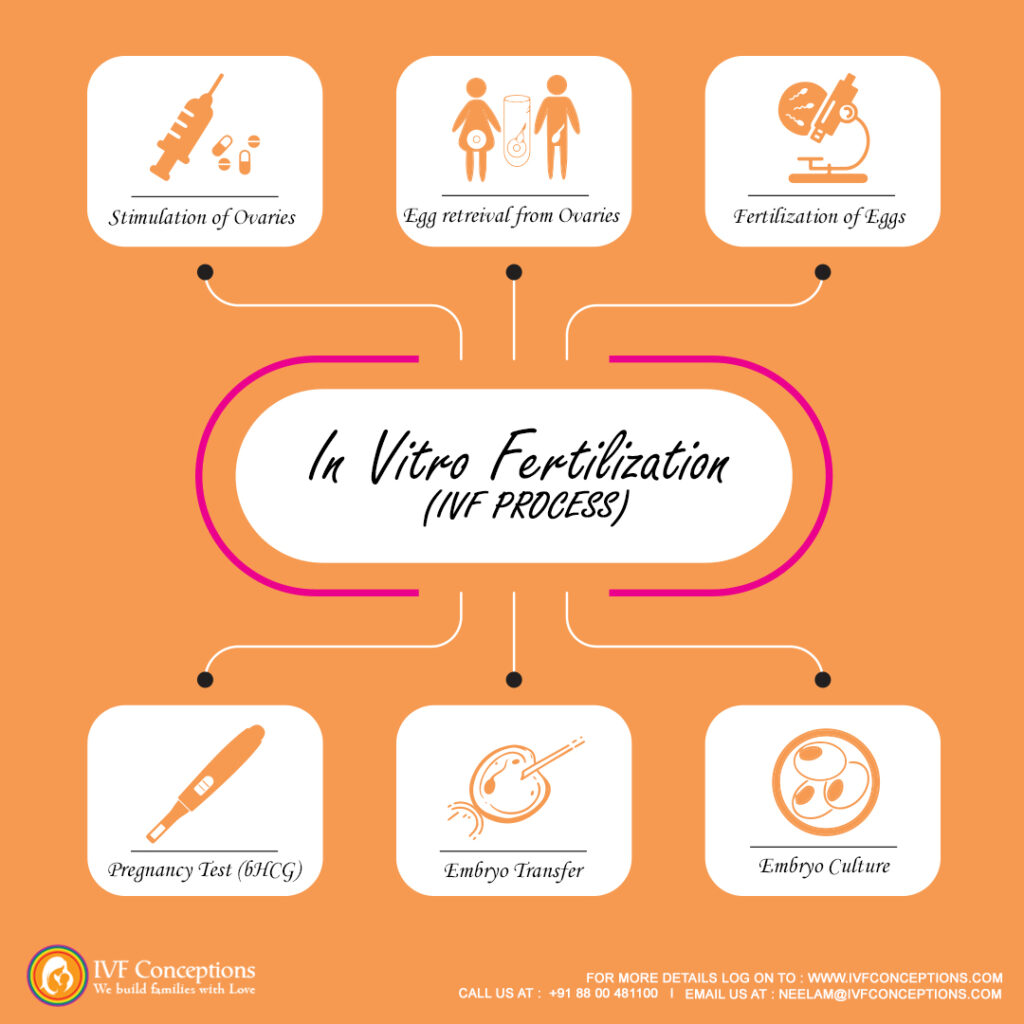
🔄 Key Steps:
- Ovarian stimulation
- Egg retrieval
- Lab fertilization
- Embryo culture
- Embryo transfer
- Pregnancy confirmation via beta hCG test
👉 Used for: tubal infertility, male factor infertility, unexplained infertility, or endometriosis.
What is IVF with Genetic Testing (PGT)?
IVF with genetic testing, also called PGT (Preimplantation Genetic Testing), is an advanced form of IVF where embryos are screened for chromosomal or genetic abnormalities before implantation.
🧬 Types of PGT:
- PGT-A (Aneuploidy Testing): Screens for extra/missing chromosomes
- PGT-M (Monogenic Testing): Detects specific inherited genetic conditions (e.g., cystic fibrosis, BRCA)
- PGT-SR (Structural Rearrangement): For known chromosomal translocations or inversions
👉 Used for: recurrent miscarriages, failed IVF, known genetic conditions, advanced maternal age
The Role of Genetic Testing in Enhancing Embryo Health
For many hopeful parents, embryo health becomes a central focus when navigating fertility treatments. Advanced screening methods now offer deeper insights into potential challenges, helping families make confident choices aligned with their goals.
Screening for Chromosomal Abnormalities
Chromosomal irregularities occur naturally but can impact embryo development. Testing analyzes cells from early-stage embryos to detect issues like Down syndrome. This process identifies which options have the highest likelihood of leading to a healthy pregnancy.
Conditions such as cystic fibrosis or structural chromosome errors are often detectable through this method. Clinics typically perform biopsies at the blastocyst stage, removing a few cells without harming the embryo’s growth potential.
Reducing the Risk of Miscarriage and Hereditary Disorders
Studies show that selecting embryos without chromosomal abnormalities may lower miscarriage risks by up to 50%. By excluding those with detectable flaws, clinics aim to improve outcomes while reducing emotional strain.
“Screening provides clarity,” notes one fertility specialist. “Families gain peace of mind knowing they’ve prioritized the healthiest possible start.” This approach also helps prevent passing on hereditary conditions linked to specific gene mutations.
While no method guarantees success, combining thorough analysis with medical expertise creates a clearer path forward. For those weighing options, understanding these benefits supports informed, personalized decisions.
Success Rates: IVF vs IVF with PGT
| Age Group | IVF Success (No PGT) | IVF with PGT-A Success |
| <35 | 45–55% | 65–75% |
| 35–39 | 30–40% | 60–70% |
| 40+ | 10–25% | 50–60% |
💡 PGT does not improve embryo quality—it improves selection accuracy.
IVF Vs IVF with genetic testing: A Comprehensive Comparison
Choosing between fertility treatment paths often feels overwhelming. Both approaches share core steps but differ in critical ways that affect outcomes, timelines, and emotional demands. Understanding these distinctions helps align your choice with personal priorities.
Pros and Cons of Each Approach
The standard approach offers simplicity and lower upfront costs. However, it provides limited insights into embryo health. Key advantages include:
- Shorter timelines (no waiting for test results)
- Reduced financial burden
- Fewer laboratory procedures
Adding advanced screening introduces new considerations. Benefits often cited by clinics include:
- Higher implantation rates (studies suggest up to 20% improvement)
- Lower risk of miscarriage from chromosomal issues
- Identification of specific genetic concerns
Trade-offs involve extended treatment cycles and costs averaging 30-50% higher. Some families also face ethical questions about embryo selection criteria.
Which Option Fits Your Fertility Journey?
Prioritizing successful pregnancy odds might lean toward screened embryos, especially for those over 35 or with hereditary conditions. Conversely, time-sensitive plans or budget constraints could favor the traditional route.
“Every family’s definition of success differs,” notes Dr. Lisa Morgan, a reproductive endocrinologist. “Some value maximizing first-attempt viability, while others prefer minimizing medical interventions.”
Consider creating a decision checklist:
- Medical history (recurrent miscarriages, known genetic risks)
- Financial flexibility
- Comfort with extended timelines
This clarity can ease decision-making, ensuring your path reflects both practical realities and heartfelt priorities.
Pros and Cons Analysis of Preimplantation Genetic Techniques
Modern fertility advancements present families with complex choices about balancing medical benefits and practical realities. Evaluating preimplantation genetic techniques requires weighing tangible improvements against logistical challenges.

Advantages: Improved Success Rates and Informed Decisions
Advanced screening helps identify embryos with the best developmental potential. By filtering out those with chromosomal disorders, clinics report up to 65% higher success rates per transfer cycle. This precision reduces multiple transfer attempts and emotional strain.
Comprehensive genetic profiles enable tailored decisions. Families gain clarity about embryo health, allowing them to prioritize options with a lower risk of complications. “This method transforms guesswork into strategy,” explains a 2023 clinical study.
Limitations: Cost, Time, and Potential Risks
Adding screening extends the treatment timeline by 2-3 weeks due to biopsy and lab analysis. Costs rise significantly, with prices ranging from $4,000 to $7,000 beyond standard procedure fees. Insurance coverage remains limited in most states.
While rare, embryo biopsy carries a 0.1% risk of damage. Some ethical debates question the selection criteria for “ideal” embryos. These factors require careful discussion with medical providers.
| Factor | Advantage | Limitation |
|---|---|---|
| Success Rate | 65% higher live birth chances | Depends on embryo quantity/quality |
| Cost | Reduces repeat cycles | Adds $4k-$7k upfront |
| Time | Single-transfer efficiency | 3-week delay for results |
| Risks | Lowers miscarriage risk | Minimal biopsy hazards |
This balanced approach helps families align their priorities—whether maximizing chances of success or managing budget constraints. Consultations with specialists remain vital for personalized planning.
Who Should Consider IVF with Genetic Testing?
IVF with PGT is recommended for:
- Women over 35–40 with increased aneuploidy risk
- Couples with recurrent miscarriage or implantation failure
- Known carriers of genetic diseases (e.g., thalassemia, BRCA)
- Couples using donor eggs or sperm
- LGBTQ+ couples via surrogacy want to transfer the healthiest embryo
Cost Considerations and Insurance Factors in the United States
Navigating fertility treatment costs requires careful planning and awareness of available resources. Prices vary widely depending on clinic location, technology used, and individual health needs. Understanding these variables helps families create realistic budgets while exploring financial support options.
Cost Comparison for IVF vs IVF with Genetic Testing
| Treatment | Average Cost (USD) |
|---|---|
| IVF (without PGT) | $10,000 – $15,000 |
| IVF with PGT-A | $15,000 – $22,000 |
| Additional Cost per Embryo | $300 – $600 |
Understanding Testing and Treatment Expenses
A standard lab-based fertilization cycle averages $12,000–$15,000. Adding chromosomal analysis increases costs by $3,000–$7,000, depending on the number of embryos tested. Some clinics charge per embryo, while others offer flat rates for groups of five or more.
Advanced screening often involves multiple fees:
- Biopsy procedure: $1,500–$2,500
- Lab analysis: $2,000–$4,500
- Storage for re-testing: $300–$600 annually
Additional Resources to read:
How To Choose Between IVF and IUI
IVF With Egg Donor Success Rates
What is Mitochondrial Donation IVF Treatment
Conclusion
Choosing between IVF and IVF with genetic testing depends on several factors—your age, fertility history, genetic risk, and emotional readiness. While standard IVF is effective for many, IVF with PGT offers an added layer of assurance and precision.
For couples with recurrent failures, older age, or known genetic concerns, IVF with genetic screening is often the recommended path toward a healthy baby and peace of mind.
💫 Why Intended Parents Choose Complete Surrogacy for a Safe, Smooth & Successful Surrogacy Journey:
🌍 Access to multiple surrogacy destinations with 15+ years of international experience
🏥 Partnerships with top-tier fertility clinics and agencies, backed by references from past clients
👩🦱 Diverse egg donor options: Asian, Caucasian, African, Oriental, and more
💸 Transparent and affordable pricing—direct payments with no extra agency fees
🔒 No hidden costs—all charges are agreed upon upfront
🤝 Dedicated case manager for personalized support
📲 Fast, honest, and clear communication throughout
📑 Full legal support for visas, documentation, and baby exit processes
🚚 Assistance with frozen sperm/embryo shipment logistics
FAQs for IVF Vs IVF with genetic testing
How does preimplantation genetic testing improve pregnancy success?
Can genetic testing prevent hereditary conditions like cystic fibrosis?
What are the main drawbacks of adding genetic screening to IVF?
Is IVF with genetic testing recommended for all patients?
No. It’s typically advised for those over 35, couples with recurrent pregnancy loss, or families with known genetic disorders. Younger patients without these factors may opt for standard IVF to reduce expenses.
How accurate are embryo biopsies in detecting abnormalities?
Modern techniques like next-generation sequencing (NGS) have over 98% accuracy for identifying chromosomal issues. However, false positives/negatives can occur, so confirmatory prenatal testing is still recommended.
Does insurance cover IVF with preimplantation testing?
Coverage varies widely. Only 18 states mandate IVF insurance, and genetic testing is often excluded. Many clinics offer financing plans or grants to help manage out-of-pocket costs.
What ethical concerns surround embryo genetic screening?
How do clinics decide which embryos to test?

Author Bio: Neelam Chhagani is an International Surrogacy Expert with 15 years of experience in the fertility and surrogacy domain. As the founder of IVF Conceptions and Complete Surrogacy, she has guided over 4,000 intended parents worldwide on their surrogacy journey to parenthood. Recognized as a trusted authority, she specializes in holistic infertility solutions and third-party reproduction consulting.
Holding an MA in Counselling Psychology and a PGD in Mental Health, Neelam is a proud member of the European Fertility Society (EFS) and the European Society of Human Reproduction and Embryology (ESHRE). She is also a leading surrogacy blogger, providing valuable insights into ethical and practical surrogacy solutions.
Since 2010, committed to supporting ALL family types, Neelam has been passionate about helping intended parents grow their families with compassion, integrity, and a focus on secure and affordable surrogacy options Globally.
Learn more about Neelam:
https://www.ivfconceptions.com/neelam-chhagani-surrogacy-consultant/
https://www.linkedin.com/in/neelam-chhagani-92892229/















I was introduced to Neelam by a friend who worked with Neelam for surrogacy. Neelam is absolutely wonderful. I am a single male and the journey to fatherhood is not that easy. Neelam connected me to a program ideal for my circumstances. She was with me throughout the pregnancy providing advice and guidance along the way. I am so grateful I found her and am thrilled today that I have a beautiful daughter. I highly recommend Neelam to anyone who is on a journey to become a parent. Having a child has changed my world for the better. I wish others success with their own journey and recommend you connect with Neelam to find a path that is best for you.
SA (USA)